
- Current
- Browse
- Collections
-
For contributors
- For Authors
- Instructions to authors
- Article processing charge
- e-submission
- For Reviewers
- Instructions for reviewers
- How to become a reviewer
- Best reviewers
- For Readers
- Readership
- Subscription
- Permission guidelines
- About
- Editorial policy
Search
- Page Path
- HOME > Search
- Metabolic Risk/Epidemiology
- A Comparison of Predictive Performances between Old versus New Criteria in a Risk-Based Screening Strategy for Gestational Diabetes Mellitus
- Subeen Hong, Seung Mi Lee, Soo Heon Kwak, Byoung Jae Kim, Ja Nam Koo, Ig Hwan Oh, Sohee Oh, Sun Min Kim, Sue Shin, Won Kim, Sae Kyung Joo, Errol R. Norwitz, Souphaphone Louangsenlath, Chan-Wook Park, Jong Kwan Jun, Joong Shin Park
- Diabetes Metab J. 2020;44(5):726-736. Published online April 13, 2020
- DOI: https://doi.org/10.4093/dmj.2019.0126
- 6,622 View
- 123 Download
- 9 Web of Science
- 9 Crossref
-
 Abstract
Abstract
 PDF
PDF Supplementary Material
Supplementary Material PubReader
PubReader  ePub
ePub Background The definition of the high-risk group for gestational diabetes mellitus (GDM) defined by the American College of Obstetricians and Gynecologists was changed from the criteria composed of five historic/demographic factors (old criteria) to the criteria consisting of 11 factors (new criteria) in 2017. To compare the predictive performances between these two sets of criteria.
Methods This is a secondary analysis of a large prospective cohort study of non-diabetic Korean women with singleton pregnancies designed to examine the risk of GDM in women with nonalcoholic fatty liver disease. Maternal fasting blood was taken at 10 to 14 weeks of gestation and measured for glucose and lipid parameters. GDM was diagnosed by the two-step approach.
Results Among 820 women, 42 (5.1%) were diagnosed with GDM. Using the old criteria, 29.8% (
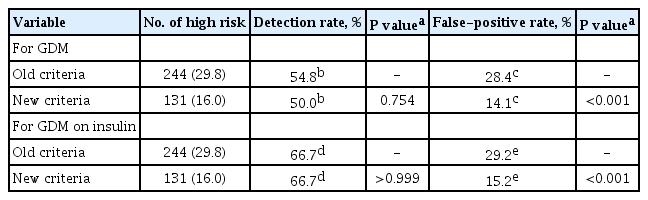
n =244) of women would have been identified as high risk versus 16.0% (n =131) using the new criteria. Of the 42 women who developed GDM, 45.2% (n =19) would have been mislabeled as not high risk by the old criteria versus 50.0% (n =21) using the new criteria (1-sensitivity, 45.2% vs. 50.0%,P >0.05). Among the 778 patients who did not develop GDM, 28.4% (n =221) would have been identified as high risk using the old criteria versus 14.1% (n =110) using the new criteria (1-specificity, 28.4% vs. 14.1%,P <0.001).Conclusion Compared with the old criteria, use of the new criteria would have decreased the number of patients identified as high risk and thus requiring early GDM screening by half (from 244 [29.8%] to 131 [16.0%]).
-
Citations
Citations to this article as recorded by- Predicting the Risk of Insulin-Requiring Gestational Diabetes before Pregnancy: A Model Generated from a Nationwide Population-Based Cohort Study in Korea
Seung-Hwan Lee, Jin Yu, Kyungdo Han, Seung Woo Lee, Sang Youn You, Hun-Sung Kim, Jae-Hyoung Cho, Kun-Ho Yoon, Mee Kyoung Kim
Endocrinology and Metabolism.2023; 38(1): 129. CrossRef - Metabolic Dysfunction-Associated Fatty Liver Disease and Subsequent Development of Adverse Pregnancy Outcomes
Seung Mi Lee, Young Mi Jung, Eun Saem Choi, Soo Heon Kwak, Ja Nam Koo, Ig Hwan Oh, Byoung Jae Kim, Sun Min Kim, Sang Youn Kim, Gyoung Min Kim, Sae Kyung Joo, Bo Kyung Koo, Sue Shin, Errol R. Norwitz, Chan-Wook Park, Jong Kwan Jun, Won Kim, Joong Shin Park
Clinical Gastroenterology and Hepatology.2022; 20(11): 2542. CrossRef - Nonalcoholic fatty liver disease and early prediction of gestational diabetes mellitus using machine learning methods
Seung Mi Lee, Suhyun Hwangbo, Errol R. Norwitz, Ja Nam Koo, Ig Hwan Oh, Eun Saem Choi, Young Mi Jung, Sun Min Kim, Byoung Jae Kim, Sang Youn Kim, Gyoung Min Kim, Won Kim, Sae Kyung Joo, Sue Shin, Chan-Wook Park, Taesung Park, Joong Shin Park
Clinical and Molecular Hepatology.2022; 28(1): 105. CrossRef - Nonalcoholic fatty liver disease-based risk prediction of adverse pregnancy outcomes: Ready for prime time?
Seung Mi Lee, Won Kim
Clinical and Molecular Hepatology.2022; 28(1): 47. CrossRef - Postprandial Free Fatty Acids at Mid-Pregnancy Increase the Risk of Large-for-Gestational-Age Newborns in Women with Gestational Diabetes Mellitus
So-Yeon Kim, Young Shin Song, Soo-Kyung Kim, Yong-Wook Cho, Kyung-Soo Kim
Diabetes & Metabolism Journal.2022; 46(1): 140. CrossRef - Effect of Different Types of Diagnostic Criteria for Gestational Diabetes Mellitus on Adverse Neonatal Outcomes: A Systematic Review, Meta-Analysis, and Meta-Regression
Fahimeh Ramezani Tehrani, Marzieh Saei Ghare Naz, Razieh Bidhendi-Yarandi, Samira Behboudi-Gandevani
Diabetes & Metabolism Journal.2022; 46(4): 605. CrossRef - Development of early prediction model for pregnancy-associated hypertension with graph-based semi-supervised learning
Seung Mi Lee, Yonghyun Nam, Eun Saem Choi, Young Mi Jung, Vivek Sriram, Jacob S. Leiby, Ja Nam Koo, Ig Hwan Oh, Byoung Jae Kim, Sun Min Kim, Sang Youn Kim, Gyoung Min Kim, Sae Kyung Joo, Sue Shin, Errol R. Norwitz, Chan-Wook Park, Jong Kwan Jun, Won Kim,
Scientific Reports.2022;[Epub] CrossRef - The Clinical Characteristics of Gestational Diabetes Mellitus in Korea: A National Health Information Database Study
Kyung-Soo Kim, Sangmo Hong, Kyungdo Han, Cheol-Young Park
Endocrinology and Metabolism.2021; 36(3): 628. CrossRef - The risk of pregnancy‐associated hypertension in women with nonalcoholic fatty liver disease
Young Mi Jung, Seung Mi Lee, Subeen Hong, Ja Nam Koo, Ig Hwan Oh, Byoung Jae Kim, Sun Min Kim, Sang Youn Kim, Gyoung Min Kim, Sae Kyung Joo, Sue Shin, Errol R. Norwitz, Chan‐Wook Park, Jong Kwan Jun, Won Kim, Joong Shin Park
Liver International.2020; 40(10): 2417. CrossRef
- Predicting the Risk of Insulin-Requiring Gestational Diabetes before Pregnancy: A Model Generated from a Nationwide Population-Based Cohort Study in Korea
- Fracture Incidence and Risk of Osteoporosis in Female Type 2 Diabetic Patients in Korea
- Jong Kwan Jung, Hyo Jeong Kim, Hong Kyu Lee, Sang Soo Kim, Chan Soo Shin, Jin Taek Kim
- Diabetes Metab J. 2012;36(2):144-150. Published online April 17, 2012
- DOI: https://doi.org/10.4093/dmj.2012.36.2.144
- 4,258 View
- 38 Download
- 15 Crossref
-
 Abstract
Abstract
 PDF
PDF PubReader
PubReader Background There are no published data regarding fracture risk in type 2 diabetic patients in Korea. In this study, we compared the fracture incidence and risk of osteoporosis of type 2 diabetic female patients with those in a non-diabetic hypertensive cohort.
Methods The incidence of fracture in a type 2 diabetic cohort was compared with that in a non-diabetic hypertensive cohort over the course of 7 years. Female type 2 diabetic and non-diabetic hypertensive patients who visited Eulji General Hospital outpatient clinic from January 2004 to April 2004 were assigned to the diabetic cohort and the non-diabetic hypertensive cohort, respectively. Surveys on fracture event, use of anti-osteoporosis medications, and bone mineral density were performed.
Results The number of fractures was 88 in the female diabetic cohort (
n =1,268, 60.6±11.5 years) and 57 in the female non-diabetic hypertensive cohort (n =1,014, 61.4±11.7 years). The RR in the diabetic cohort was 1.38 (P =0.064; 95% confidence interval [CI], 0.98 to 1.94) when adjusted for age. Diabetic patients with microvascular complications (61.0%) showed a higher RR of 1.81 (P =0.014; 95% CI, 1.13 to 2.92) compared with those without these complications. The prevalence of osteoporosis was comparable between the groups, while use of anti-osteoporosis medication was more common in the diabetic cohort (12.8%) than in the hypertensive cohort (4.5%) (P <0.001).Conclusion In our study, a higher fracture risk was observed in female type 2 diabetics with microvascular complications. Special concern for this risk group is warranted.
-
Citations
Citations to this article as recorded by- Research Progress on How to Prevent Osteoporosis in Diabetic Patients
婷玉 牛
Advances in Clinical Medicine.2022; 12(02): 1178. CrossRef - Differences in the roles of types 1 and 2 diabetes in the susceptibility to the risk of fracture: a systematic review and meta-analysis
Jiaqing Dou, Jing Wang, Qiu Zhang
Diabetology & Metabolic Syndrome.2021;[Epub] CrossRef - The risk of hip and non-vertebral fractures in type 1 and type 2 diabetes: A systematic review and meta-analysis update
Tatiane Vilaca, Marian Schini, Susan Harnan, Anthea Sutton, Edith Poku, Isabel E. Allen, Steven R. Cummings, Richard Eastell
Bone.2020; 137: 115457. CrossRef - Diabetes mellitus and risk of low-energy fracture: a meta-analysis
Jing Bai, Qian Gao, Chen Wang, Jia Dai
Aging Clinical and Experimental Research.2020; 32(11): 2173. CrossRef - Diabetes mellitus and the risk of fractures at specific sites: a meta-analysis
Hao Wang, Ying Ba, Qian Xing, Jian-Ling Du
BMJ Open.2019; 9(1): e024067. CrossRef - The use of metformin, insulin, sulphonylureas, and thiazolidinediones and the risk of fracture: Systematic review and meta‐analysis of observational studies
Khemayanto Hidayat, Xuan Du, Meng‐Jiao Wu, Bi‐Min Shi
Obesity Reviews.2019; 20(10): 1494. CrossRef - Bei Diabetikern an eine Osteoporose denken!
Stephan Scharla
MMW - Fortschritte der Medizin.2018; 160(21-22): 65. CrossRef - Type 2 diabetes and risk of low-energy fractures in postmenopausal women: meta-analysis of observational studies
Joanna Dytfeld, Michał Michalak
Aging Clinical and Experimental Research.2017; 29(2): 301. CrossRef - Risk of low-energy fracture in type 2 diabetes patients: a meta-analysis of observational studies
P. Jia, L. Bao, H. Chen, J. Yuan, W. Liu, F. Feng, J. Li, H. Tang
Osteoporosis International.2017; 28(11): 3113. CrossRef - Comorbidity and its relationship with health service use and cost in community-living older adults with diabetes: A population-based study in Ontario, Canada
Kathryn Fisher, Lauren Griffith, Andrea Gruneir, Dilzayn Panjwani, Sima Gandhi, Li (Lisa) Sheng, Amiram Gafni, Patterson Chris, Maureen Markle-Reid, Jenny Ploeg
Diabetes Research and Clinical Practice.2016; 122: 113. CrossRef - Type 2 diabetes mellitus and bone fragility: Special focus on bone imaging
Yong Jun Choi, Yoon-Sok Chung
Osteoporosis and Sarcopenia.2016; 2(1): 20. CrossRef - Epidemiology of fractures in type 2 diabetes
Ann V. Schwartz
Bone.2016; 82: 2. CrossRef - Efficacy and Safety of Weekly Alendronate Plus Vitamin D35600 IU versus Weekly Alendronate Alone in Korean Osteoporotic Women: 16-Week Randomized Trial
Kwang Joon Kim, Yong-Ki Min, Jung-Min Koh, Yoon-Sok Chung, Kyoung Min Kim, Dong-Won Byun, In Joo Kim, Mikyung Kim, Sung-Soo Kim, Kyung Wan Min, Ki Ok Han, Hyoung Moo Park, Chan Soo Shin, Sung Hee Choi, Jong Suk Park, Dong Jin Chung, Ji Oh Mok, Hong Sun Ba
Yonsei Medical Journal.2014; 55(3): 715. CrossRef - Increased Risk of Fracture and Postfracture Adverse Events in Patients With Diabetes: Two Nationwide Population-Based Retrospective Cohort Studies
Chien-Chang Liao, Chao-Shun Lin, Chun-Chuan Shih, Chun-Chieh Yeh, Yi-Cheng Chang, Yuan-Wen Lee, Ta-Liang Chen
Diabetes Care.2014; 37(8): 2246. CrossRef - Aortic Calcification and Bone Metabolism: The Relationship between Aortic Calcification, BMD, Vertebral Fracture, 25-Hydroxyvitamin D, and Osteocalcin
Kwang Joon Kim, Kyoung Min Kim, Kyeong Hye Park, Han Seok Choi, Yumie Rhee, Yong Ho Lee, Bong Soo Cha, Myong Jin Kim, Sun Min Oh, J. Keenan Brown, Sung Kil Lim
Calcified Tissue International.2012; 91(6): 370. CrossRef
- Research Progress on How to Prevent Osteoporosis in Diabetic Patients
- Relationship of Insulin-like Growth Factor(IGF)-1, IGF-2, IGF Binding Protein(IGFBP)-3, and Mitochondrial DNA Amount in the Umbilical Cord Blood to Birth Weight.
- Yun Yong Lee, Do Joon Park, Chan Soo Shin, Kyong Soo Park, Hong Kyu Lee, Jong Kwan Jun, Boh Yun Yoon, Jih Yeun Song, Bong Sun Kang
- Korean Diabetes J. 1999;23(1):36-45. Published online January 1, 2001
- 932 View
- 17 Download
-
 Abstract
Abstract
 PDF
PDF - BACKGROUND
Reaven proposed a syndrome (syndrome X), consisting of glucose intolerance, hypertension, hyperinsulinemia, dyslipidemia, as a clinical entity. The fundamental metabolic defect of this syndrome was recognized as insulin resistance, but the pathophysiology of insulin resistance is not clarified as of yet. Recent evidence, suggests that non-insulin dependent diabetes mellitus (NIDDM) ancl lipid and cardiovascular abnormalities-syndrome X-are associated with intrauterine growth retar- dation (IUGR). Recently Shin reported that the amounts of mitochondrial DNA (mtDNA) in a given amount of genomic DNA were lower in NIDDM patients than in healthy controls, and the amount of mtDNA is negatively correlated with blood pressure ancl waist-hip ratio. Birth weight is known to be correlated with levels of insulin-like growth factors (IGFs). The purpose of this study was to identify the correlation of low birth weight with reduced mtDNA and syndrome X. We investigated the relationship of birth weight to IGFs and the amount of mtDNA METHODS: 72 singleton pregnancy babies and their mathers admitted in Seoul National University Hospital from March to May, 1997 were studied. After delivery, the cord blcxxl and maternal venous blood sampling was done. Using the imnnmoradiometric assay (IRMA) the IGF-l, IGF-2, IGFBP-3 was measured from cord and maternal plasma. Among them only 27 pairs samples were measured mtDNA amount with competitive PCR method in their buffy coat. Then statistical analysis was done within these paratneters. RESULTS: Birth weight is correlated significantly with cord plasma IGF-1 (r=0.32, p<0.01), IGFBP-3 (r=0.44, p<0.01), prepregnancy maternal body weight (r=0.45, p<0.01), maternal mtDNA amount (r=0.63, p<0.01). Cord blood mtDNA is correlated with maternal mtDNA amount (r=0.55, p<0,01). In multiple regression analysis, the maternal mtDNA was found to be the only independent factor related to birth weight (p<0.01). COMCLUSION: We have found the correlation between birth weight and maternal prepregnancy body weight and mtDNA amount. The clinical implications of this result remain yet to be deiermined.

 KDA
KDA
 First
First Prev
Prev





